Preserving Photoreceptors Following Retinal Injury
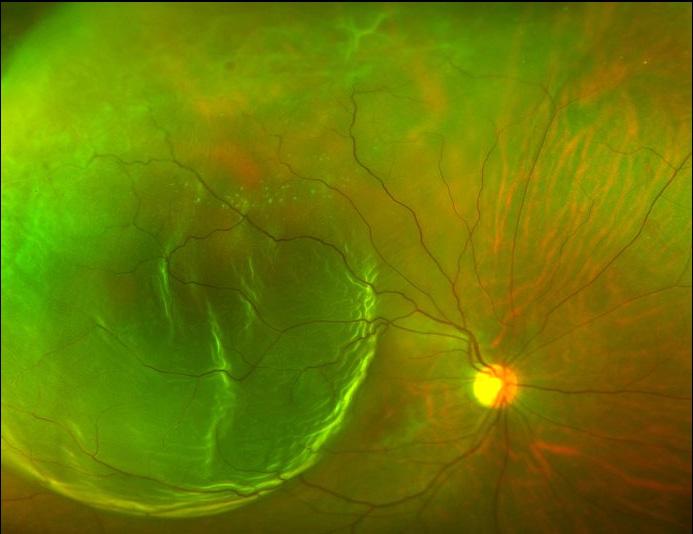
A representative color fundus photograph in right eye of a patient with a superotemporal bullous retinal detachment with a superior micro hole. (Image was kindly provided by Ryo Mukai, Gunma University Hospital, Maebashi, Japan.)
RPB-supported vision researchers have identified targets for treatments that would prevent vision loss in patients following retinal detachment. The discovery holds promise for the many patients who, even though they have corrective surgery soon after experiencing a retinal detachment, continue to lose sight.
The research shows, for the first time, that a component of the body's immune system called the alternative complement pathway significantly contributes to photoreceptor cell death and that inhibiting the pathway is protective.

Perceived visual field of an individual with a retinal detachment. In an individual with a retinal detachment the retina becomes separated from its underlying support tissue. In the area of the detachment, vision is lost (black area in the right panel). The area of vision loss depends on the size of the initial detachment. If left untreated the detachment can progress leading to an even larger field of loss and eventual loss of all vision. Patients describe this effect like the closing of a shutter. The appearance of "floaters" is also common, which patients perceive as globs or strands floating in their field of vision. Based on the degree and or location of the retinal detachment, some individuals experience blurred vision in their remaining visual field unaffected by the detachment. (Image courtesy of Dr. Eiichi Hasagawa (Massachusetts Eye and Ear Infirmary) and retinal detachment visual field representation is courtesy of Kristin Johnson (Boston Children's Hospital).
Ultimately, the findings may have much broader impact, because degeneration of photoreceptors also occurs as a result of blunt trauma or as a side effect of a variety of diseases including retinopathy of prematurity, diabetic retinopathy, ocular tumors, and age-related macular degeneration.
Q&A with Kip M. Connor, Ph.D.
Q&A with Kip M. Connor, Ph.D., Assistant Professor of Ophthalmology at Mass. Eye and Ear/HMS Ophthalmology, RPB Special Scholar Award recipient and lead author on the study.
What is the main finding in your study? Why is it novel?
Retinal detachment and subsequent degeneration of the retina can lead to progressive visual decline due to photoreceptor cell death, the major light-sensing cell in the eye. The detached photoreceptors begin to die, and given that photoreceptors are non-dividing cells, their loss leads to irreversible visual impairment even after successful retinal reattachment surgery. Early inflammatory mediators are up regulated in the eyes of these patients; of particular interest are those of the alternative complement pathway. For the first time these results provide evidence that the alternative complement pathway exacerbates photoreceptor cell death and that inhibition of the pathway is protective.
How did you conduct the experiment(s)?
To better understand the underlying disease mechanisms we analyzed innate immune system regulators in the vitreous of human patients with retinal detachment. In an experimental model, we identified the alternative complement pathway as promoting early photoreceptor cell death during retinal detachment. Interestingly, injured photoreceptors lose proteins that normally protect them from complement mediated cell death, allowing for selective targeting by the alternative complement pathway. Lastly, we found that by blocking the alternative complement pathway, through both genetic and pharmacologic means, photoreceptors were protected from cell death.
What are the clinical implications of your finding(s)?
Degeneration of photoreceptors is a primary cause of vision loss worldwide, making the underlying mechanisms surrounding photoreceptor cell death critical to developing new treatment strategies. It occurs as a result of either blunt trauma or a side effect of a variety of diseases including retinopathy of prematurity, diabetic retinopathy (tractional RD), ocular tumors, and age-related macular degeneration (exudative RD). The current standard of care involves surgical reattachment, which is typically provided within a week in the US and Europe. While surgery has proven to be highly effective at reattaching the retina, speed is critical to a positive outcome. This is due to the fact that increased severity and duration of the detachment results in a significant decrease in overall visual regeneration. Unfortunately, even when reattachment is performed in a timely manner, patients often complain of permanent vision loss accompanied by changes in color vision. Visual acuity only improves to 20/50 in 39% of patients, even when early reattachment surgery is performed. Importantly, studies in both humans and animal models have shown that photoreceptor cell death is induced as early as 12 hours after RD. This indicates that early intervention could potentially preserve the photoreceptors, improving the visual acuity of patients that undergo both early and late stage reattachment procedures. Our data provides a new role for complement in retinal detachment, and suggests that complement inhibitors may be good therapeutic targets to prevent the initial photoreceptor cell loss, providing an extended therapeutic window for surgery and photoreceptor survival.
Outside of the main finding(s), does this study suggest exciting ideas, concepts, etc. that might be of interest to a general audience?
The idea of the innate immune system targeting and removing only damaged/injured cells, while leaving the surrounding healthy cells intact, introduces an overarching concept for the role of the innate immune system in disease. The complement system consists of serum and tissue proteins, membrane-bound receptors, and a number of regulatory proteins, forming a hub-like network that is tightly connected to other systems; the three key pathways are: the classical, lectin, and alternative pathways. Damaged or diseased host cells down-regulate membrane-bound inhibitors of complement, allowing for targeted clearance. An imbalance between complement recognition and initiation on healthy host cells can lead to unregulated complement activation and subsequent cellular damage. The complement system is likely to be a critical component of ocular immunity, but in the context of photoreceptor survival after injury this selective targeting is deleterious, likely leading to increased visual decline.
"Our findings begin to identify a new role of the innate immune system by which the body's internal mediators selectively target injured detached photoreceptors for removal," says Kip M. Connor, Ph.D., Assistant Professor of Ophthalmology at Mass. Eye and Ear/HMS Ophthalmology and an RPB Special Scholar Award recipient. "It is our hope that future studies will allow us to develop specific therapeutics that harness this knowledge resulting in a greater visual outcome and quality of life for patients suffering from this sight threatening disease."
July 23, 2015
Related News: Top Story

New study shows that diabetic eye disease is up, but the most severe forms are down
Data from an RPB and MTMVI-supported study showed that while diabetes-related eye diseases doubled since 2014, the most severe forms of the disease have decreased.

RPB Hosts Vision Research Funding Partnership 2025
Leaders of organizations that fund vision research convened in Washington, D.C. to increase collaboration and maximize the impact of research funding for sight-threatening diseases.

Research to Prevent Blindness Celebrates 65 Years of Success
Since 1960, RPB has been transforming vision research and eyecare for the benefit of all people

Research to Prevent Blindness and Association of University Professors of Ophthalmology Announce 2025 Recipient of RPB David F. Weeks Award for Outstanding Vision Research
Maria Bartolomeo Grant, MD, is recognized for ground-breaking contributions to the field of vision research.

The Time is Now to Protect the National Eye Institute
The existence of the National Eye Institute, the most important source of funding for vision research in the U.S., is being threatened.

RPB Grantees Contribute to Eye Transplantation Effort
The ARPA-H THEA project takes on an exciting challenge.
Subscribe
Get our email updates filled with the latest news from our researchers about preventing vision loss, treating eye disease and even restoring sight. Unsubscribe at any time. Under our privacy policy, we'll never share your contact information with a third party.
| General Info | Grants | News & Resources |



