RPB Funding Yields Big Gains
 Crowds at the ARVO 2013 meeting of nearly 12,000 vision scientists and physicians from around the world heard and saw the hundreds of ways that funding from Research to Prevent Blindness (RPB) is yielding major research advances for preserving vision and restoring eyesight.
Crowds at the ARVO 2013 meeting of nearly 12,000 vision scientists and physicians from around the world heard and saw the hundreds of ways that funding from Research to Prevent Blindness (RPB) is yielding major research advances for preserving vision and restoring eyesight.
RPB's presence was palpable throughout the ARVO 2013 Annual Meeting. It's newly designed logo popped everywhere -- on scientific posters and at presentations where scientists displayed their RPB-supported, cutting-edge research. The advanced nature of the work drew plenty of attention, and its creative support of the emerging imaging technology known as OCT was particularly eye catching.
The Association for Research in Vision and Ophthalmology (ARVO) is the world's premier vision research organization. The ARVO annual meeting, held this year in May in Seattle, is where researchers come to display their results in poster format, on stage, in smaller meetings and even in corners of hallways to share findings that ultimately further the goal of advancing technologies and treatments for preventing blindness. RPB attends every year to garner new information, meet with RPB-supported scientists, and engage with other leaders in the field.
Optical coherence tomography (OCT)
Highlights of the meeting included reports showing ways that RPB funding of an advanced technology called optical coherence tomography(OCT) is yielding research findings that are changing ophthalmology research and practice.
Perhaps the most groundbreaking use of OCT was presented by Ruikand (Ricky) Wang, Ph.D., who is using RPB funds to show unprecedented OCT structural and functional details of the eye. Dr. Wang is Professor of Bioengineering and Adjunct Professor in the Department of Ophthalmology at the University of Washington Eye Center and recipient of RPB's Innovative Ophthalmic Research Award, a prize inaugurated in 2011 to fund "out of the box" basic research. Winning scientists receive $100,000 to apply to their area of unique work. Dr. Wang's OCT research, called optical microangiography (OMAG) and described below, is expected to give researchers new tools for understanding the causes of several vision disorders, and how and whether new treatments under development will have a significant impact.
 "I have been privileged to be awarded an Innovative Research Award from RPB," says Dr. Wang. "It enables me to explore novel ideas that use the already proven optical coherence tomography to image functional blood perfusion through the retina, layer by layer. The ability to visualize blood flow in many layers of the retina is incredibly important because major causes of blindness in the world are due to abnormal blood circulation."
"I have been privileged to be awarded an Innovative Research Award from RPB," says Dr. Wang. "It enables me to explore novel ideas that use the already proven optical coherence tomography to image functional blood perfusion through the retina, layer by layer. The ability to visualize blood flow in many layers of the retina is incredibly important because major causes of blindness in the world are due to abnormal blood circulation."
OCT is like a sonogram except that it uses light waves instead of sound waves to capture images of normal and diseased aspects of the eye. First introduced by scientists and engineers at Massachusetts Institute of Technology in the 1990s, the still relatively new and emerging technology offers advantages over other tissue imaging processes.
OCT is non-invasive, meaning that no surgery or biopsy is involved. It is performed quickly and in real time, enabling rapid and sometimes instantaneous diagnosis and treatment. (A patient looks into a viewer and within seconds the OCT exam is complete.) It is compact enough to be portable. The output is a state-of-the-art 3D topographic map of the layers of the retina and other structures of the eye. In addition to diagnosis, OCT can be used to monitor eye disease progression and to measure responses of the eye to treatment. Its original use was for viewing layers and features, originally in 2D, but OCT is now being applied to other structures of the eye and continues to evolve as scientists unfold its potential. (For more on RPB OCT-based research, click here.)
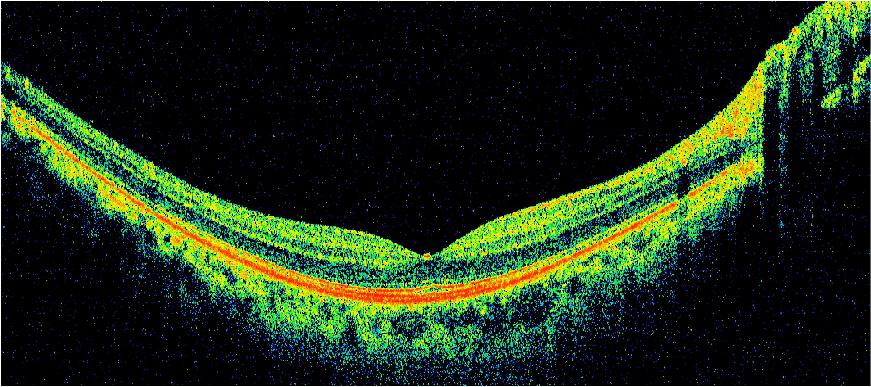
This traditional OCT image shows a cross-section of the retinal layers. The dip in the center represents the fovea, the portion of the retina responsible for sharp, central vision. Photo: Dr. Wang
Dr. Wangs work adds a new feature to existing OCT studies—a functional analysis of the eye in health and disease. Functional refers to physiological characteristics, like the rate of flow of blood through the vessels that the other versions of OCT show so remarkably but only as static structural features.
This functional work was developed by Dr. Wang and his colleagues. He believes that this novel OMAG imaging technology will become a valuable tool for investigating blood vessel involvement in eye diseases like age-related macular degeneration, diabetic retinopathy, glaucoma, and myopia, among others. Dr. Wang sat down with RPB at ARVO to discuss the remarkable gains provided by functional OCT.
OMAG for showing blood vessel activity
As Dr. Wang describes it, the retina depends on a finely organized network of tiny blood vessels for its health and survival. The retina is one of the most metabolically active organs of the body and requires adequate blood flow to supply nutrients and whisk away metabolic waste products. Even a small disruption in the retinal vasculature can lead to permanent vision loss.
Ophthalmologists often use a standard diagnostic tool called fluorescein angiography (FA) to evaluate blood vessels of the retina. While FA provides good basic images of retinal blood vessels, it has major drawbacks:
- injection of a contrast agent into the blood stream, which some patients find quite uncomfortable and sometimes elicits an allergic reaction;
- lack of detailed information about retinal vessels at variable depths; and
- FA cannot tell researchers anything about the rate of blood flow through the vessels, a unique and important benefit of OMAG.
OMAG, on the other hand, produces crisper images of blood vessels at greater depths than FA, and in 3D rather than 2D. It requires no contrast agent. And it can measure blood flow in the retina and optic nerve, right down to the passage of single blood cells through tiny capillaries.
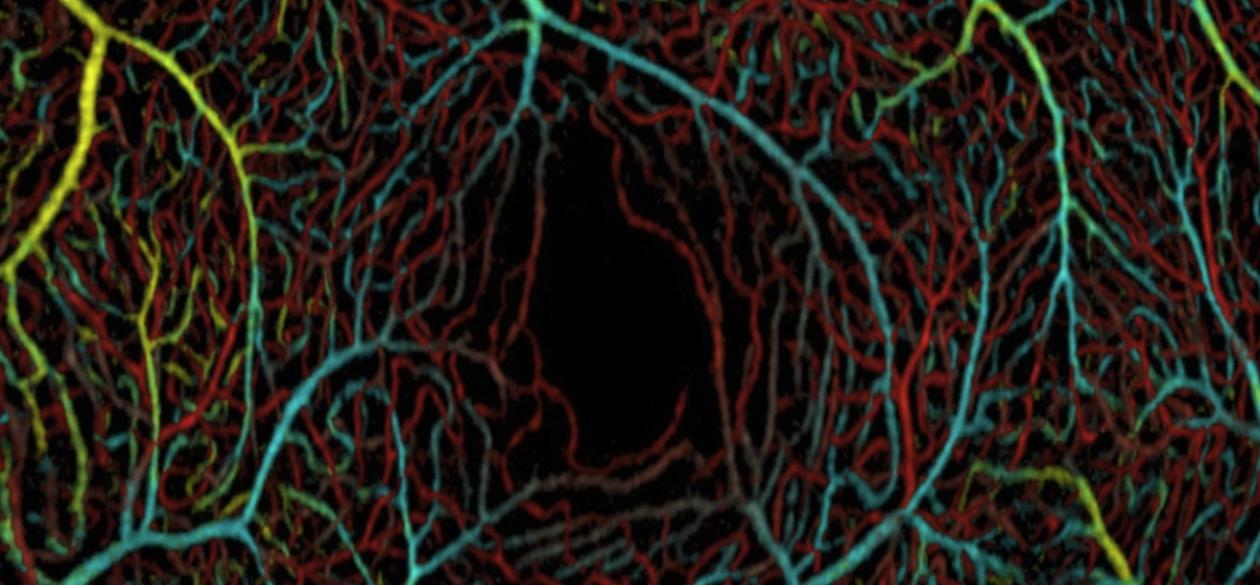
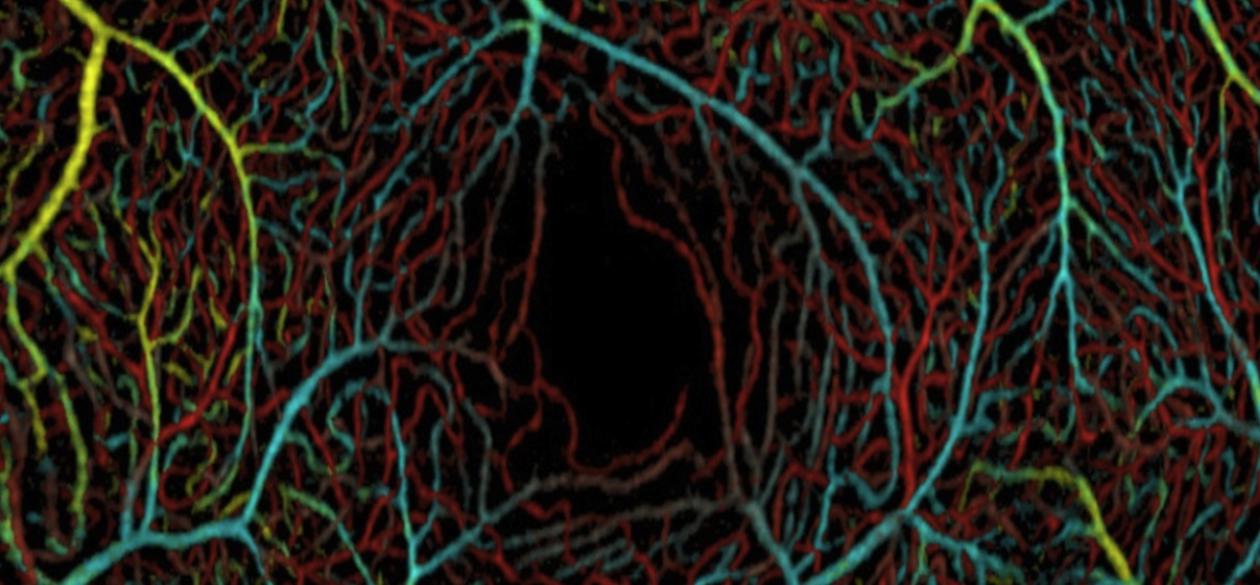
This OMAG image shows tiny blood vessels at three depths within the macula of the retina. The artificial colors correspond to vessels within the ganglion cell layer (yellow and cyan), inner plexiform layer (green), and outer plexiform layer (red). The dark zone in the lower right is a normally non-vascularized area called the fovea. Photo: Dr. Wang
Dr. Wang and his colleagues have already managed to speed up their OMAG technology in order to achieve better images and to reduce the effect of eye movement on measurements. They've also set it up so that two types of images are obtained: a large field of view for looking at large portions of the retina and optic nerve, and a crisper and smaller field of view, honing in on the blood vessels. Both modes show blood vessels at three retinal depths.
Dr. Wang is applying RPB funding, in part, for pioneering work toward understanding glaucoma, the second leading cause of blindness in the world. His lab has adapted OMAG to provide unprecedented 3D images of microscopic blood vessels of the optic nerve head (affected in glaucoma) while simultaneously recording rates of optic nerve head blood flow. This work will help identify causes of glaucomatous damage of the optic nerve, and could lead to new treatments.
At the same time, Dr. Wang and his colleagues have further adapted OCT to look at the mechanics of a structure in the front of the eye involved in glaucoma, called the trabecular meshwork. The trabecular meshwork is part of the drainage system that normally prevents build-up of fluid pressure inside the eye. They have shown for the first time that the flow from the trabecular is synchronized with the beat of the heart. They have also characterized the strength of the trabecular network and the velocity of fluid movement. This work could lead to development of a diagnostic tool for measuring failures of the drainage system and to treatments to prevent elevated intraocular pressure in glaucoma.
RPB at the Forefront
Development of OCT and optical microangiography are examples of the many areas where RPB funding is advancing knowledge and cures that will make a difference for vast numbers of people. Since 1960, RPB has distributed hundreds of millions of dollars to medical institutions to support vision scientists and research laboratories. RPB has made an impact on every aspect of ophthalmology—from the front of the eye (cornea) to the back (retina and optic nerve); for the youngest (premature babies) to the oldest patients; and in basic (molecular) to applied (artificial vision) research. RPB provides funds to over 57 leading scientific institutions in the U.S., translating into support for hundreds of the world's best and most productive researchers. In 2011 alone, these scientists made discoveries that yielded 1,322 published papers, a mark of their productivity. In 2012, they published an impressive 1,599 papers. It is no wonder that the eyes of the world are on RPB.
Elaine A. Richman, Ph.D., of Richman Associates, LLC, specializes in ophthalmology communications.
May 22, 2013
Subscribe
Get our email updates filled with the latest news from our researchers about preventing vision loss, treating eye disease and even restoring sight. Unsubscribe at any time. Under our privacy policy, we'll never share your contact information with a third party.
| General Info | Grants | News & Resources |



